Hormone Optimization Scottsdale
Physician-Supervised Hormone Replacement for Men and Women
Comprehensive hormone optimization at our Scottsdale clinic restores declining testosterone, balances thyroid function, and addresses hormonal imbalances affecting energy, body composition, cognitive function, and quality of life. This isn’t a quick prescription TRT clinic—it’s physician-supervised hormone replacement integrated into complete metabolic and cardiovascular health management. We test comprehensively, interpret results in context of overall health, prescribe bioidentical hormones when clinically appropriate, monitor regularly for effectiveness and safety, and adjust treatment based on symptoms and lab values. Hormone optimization is part of our preventative medicine approach to maintaining health and function as you age, not just isolated hormone prescription.
Comprehensive hormone testing
Testosterone (total and free), SHBG, estradiol, thyroid panel, DHEA, and other hormones affecting metabolism and aging
Bioidentical hormone replacement
Testosterone therapy for men, hormone replacement therapy for women, thyroid optimization, and DHEA supplementation when indicated
Regular monitoring and adjustment
Regular blood work tracking hormone levels, safety markers, and metabolic effects with dose adjustments based on results
Integrated health optimization
Hormone therapy combined with body composition tracking, metabolic health management, and cardiovascular risk monitoring
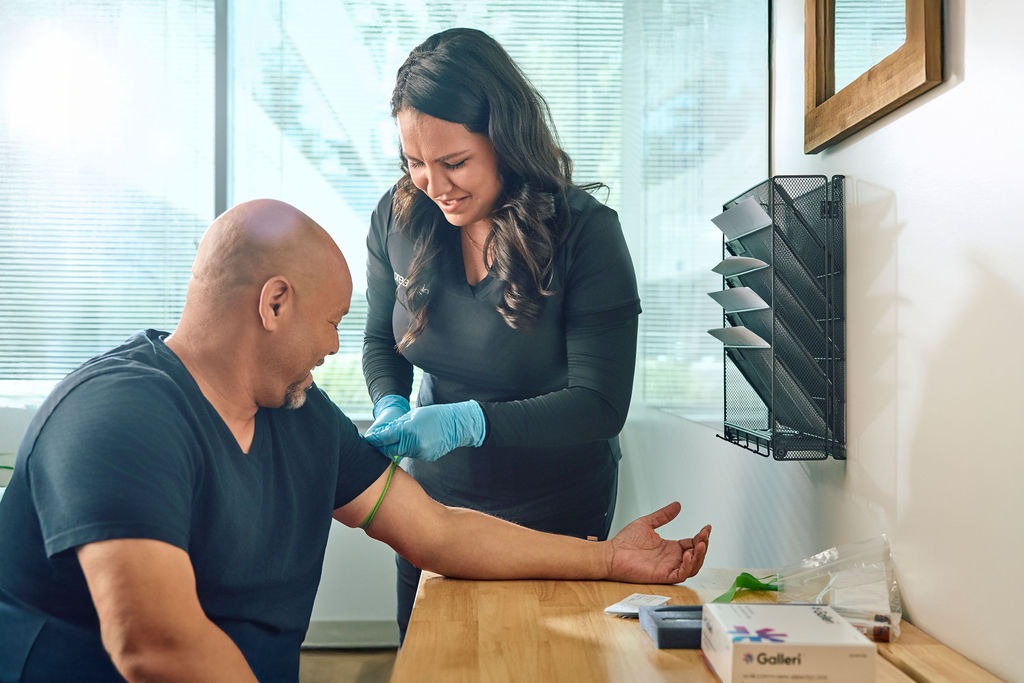
Why Consider Hormone Optimization in Scottsdale?
Hormone levels naturally decline with age—testosterone drops 1-2% annually in men after 30, women experience dramatic declines at menopause, and thyroid function often becomes suboptimal in the 40s and 50s. These declines aren’t necessarily pathological, but they cause measurable symptoms and health consequences: reduced energy and vitality, loss of muscle mass and increased body fat, declining bone density, reduced libido and sexual function, mood changes and cognitive decline, and increased metabolic dysfunction. When hormone deficiency is confirmed through testing and causing symptoms or health issues, bioidentical hormone replacement can restore function, improve quality of life, and support healthy aging. The key is proper testing, medical supervision, appropriate dosing, and regular monitoring—not DIY protocols or isolated hormone prescription without comprehensive health assessment.
HORMONE REPLACEMENT FOR WOMEN
Women experience dramatic hormone declines at menopause—estrogen, progesterone, and testosterone all drop substantially, causing hot flashes, night sweats, mood changes, fatigue, complete loss of libido, difficulty maintaining muscle, weight gain, bone density loss, and cognitive changes. Comprehensive hormone replacement therapy addressing estrogen and progesterone (if uterus is intact) alleviates many symptoms, but adding testosterone—often overlooked in standard HRT—significantly improves energy, libido, muscle maintenance, and overall vitality. Bioidentical hormone therapy tailored to individual needs and monitored regularly optimizes quality of life during and after menopause while supporting long-term bone and cardiovascular health.
TESTOSTERONE OPTIMIZATION FOR MEN
Low testosterone affects 20-40% of men over 40, causing fatigue, reduced muscle mass, increased abdominal fat, low libido, erectile dysfunction, mood changes, and cognitive decline. When testosterone is genuinely deficient (consistently below 300-400 ng/dL) and causing symptoms, testosterone replacement therapy improves energy and mood, increases muscle mass and strength, reduces body fat (particularly visceral fat), improves bone density, enhances libido and sexual function, and supports metabolic health by improving insulin sensitivity. Proper TRT requires comprehensive testing, medical supervision, regular monitoring of testosterone levels and safety markers, and integration with overall health optimization—not just prescribing testosterone in isolation.
THYROID OPTIMIZATION
Subclinical hypothyroidism and suboptimal thyroid function are common after 40, causing fatigue, weight gain, cold intolerance, brain fog, depression, and metabolic dysfunction. Standard thyroid testing (TSH only) misses many cases of thyroid dysfunction. Comprehensive thyroid assessment includes TSH, free T4, free T3, reverse T3, and thyroid antibodies, revealing subclinical hypothyroidism, poor T4 to T3 conversion, or autoimmune thyroid disease that standard testing misses. Thyroid hormone optimization—whether levothyroxine, combination T4/T3 therapy, or natural desiccated thyroid—improves energy, metabolism, cognitive function, and overall wellbeing when properly dosed and monitored.
COMPREHENSIVE HORMONE BALANCE
Hormones don't function in isolation—testosterone, estrogen, thyroid, cortisol, DHEA, and growth hormone interact in complex ways affecting metabolism, body composition, mood, and aging. Optimizing one hormone while ignoring others produces suboptimal results or creates new imbalances. Our comprehensive approach tests and addresses multiple hormonal systems, ensuring estrogen doesn't rise too high with testosterone therapy in men, thyroid function is optimized alongside sex hormones, cortisol patterns are assessed and addressed, and DHEA supplementation is considered when deficient. This integrated hormone optimization supports overall health rather than just treating isolated deficiencies.


Medical-Grade Hormone Optimization in Scottsdale
We're not a TRT mill or quick-script hormone clinic—we're physicians providing comprehensive hormone optimization integrated into preventative medicine.
Many hormone clinics prescribe testosterone after minimal testing, provide no ongoing medical supervision, ignore safety monitoring, and treat hormones in isolation from overall health. We take a different approach: comprehensive testing before treatment (not just total testosterone—free testosterone, SHBG, estradiol, full metabolic panel, cardiovascular markers, thyroid, etc.), physician evaluation ensuring hormone replacement is appropriate and safe, proper dosing achieving physiologic levels (not supraphysiologic doses), regular monitoring every 3-6 months tracking hormone levels and safety markers (hematocrit, PSA, liver function, lipids, glucose metabolism), and integration with body composition tracking, metabolic health management, and cardiovascular risk assessment. This is hormone optimization as part of comprehensive preventative care, not isolated hormone prescription.
COMPREHENSIVE TESTING
Complete hormone and metabolic assessment before treatment
We measure total testosterone, free testosterone, sex hormone-binding globulin (SHBG), estradiol, luteinizing hormone (LH), follicle-stimulating hormone (FSH), prolactin, complete thyroid panel (TSH, free T4, free T3, reverse T3, antibodies), DHEA-S, cortisol, comprehensive metabolic panel, lipid panel with advanced cardiovascular markers, PSA (for men), and other markers as clinically indicated. This comprehensive testing reveals whether hormone deficiency is present, identifies the cause (primary vs. secondary), and establishes baseline values for monitoring. We don’t prescribe hormones based on symptoms alone—we confirm deficiency through proper testing.
PHYSICIAN-SUPERVISED
Medical expertise, not wellness coaching
Our physicians have extensive training in endocrinology, metabolic medicine, and hormone replacement therapy. We interpret lab values in context of symptoms, medical history, and overall health goals. We determine appropriate dosing, monitor for effectiveness and side effects, adjust therapy based on results, and manage any complications. You’re working with actual physicians who can prescribe medications, order comprehensive testing, and provide medical supervision—not health coaches or non-physician providers operating under minimal supervision.
SAFETY MONITORING
Regular testing tracking effectiveness and potential risks
Hormone replacement requires ongoing monitoring to ensure safety and effectiveness. We check testosterone levels ensuring you’re in optimal range (not too low, not supraphysiologic), estradiol to prevent excess conversion from testosterone, hematocrit watching for polycythemia, PSA monitoring prostate health, lipid panels tracking cardiovascular effects, glucose metabolism ensuring insulin sensitivity improves, liver function if using certain formulations, and symptom assessment tracking energy, mood, libido, body composition, and quality of life. Testing every 3-6 months allows dose adjustments optimizing benefits while minimizing risks.
INTEGRATED OPTIMIZATION
Hormones as part of complete health management
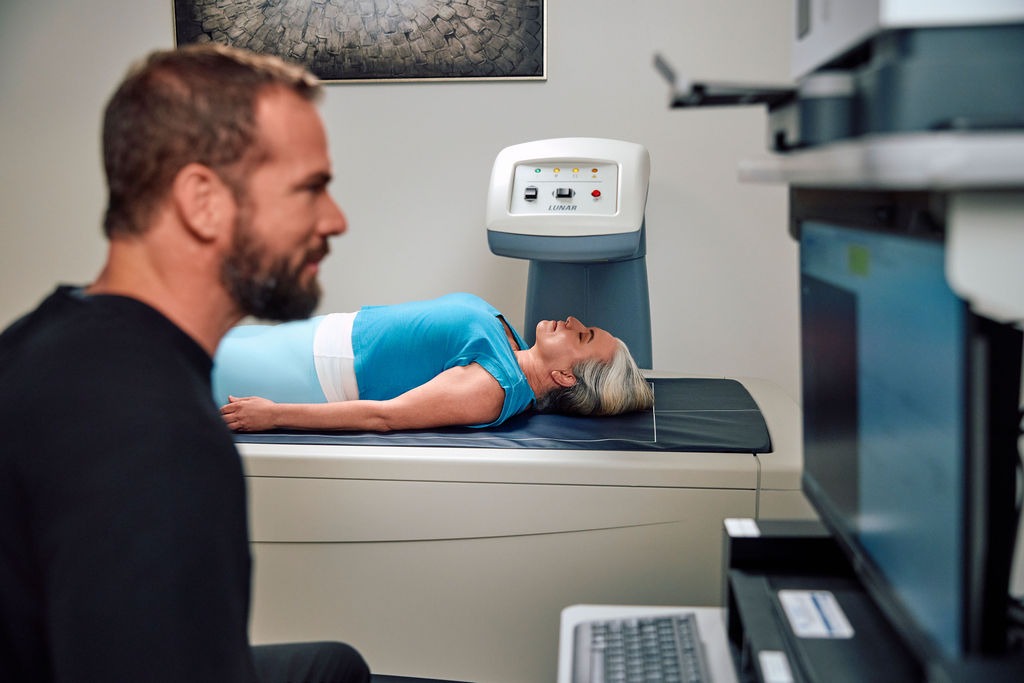
We don’t just prescribe testosterone or thyroid hormone and send you on your way. Hormone optimization is integrated with DEXA body composition tracking showing muscle gain and fat loss, metabolic biomarker monitoring ensuring insulin sensitivity improves, cardiovascular risk assessment managing lipids and inflammation, sleep optimization (critical for hormone production), nutrition and exercise guidance supporting hormone optimization goals, and medication management if you’re on other medications affecting hormones. This comprehensive approach addresses root causes and optimizes health holistically, not just hormone levels in isolation.
Hormone Optimization Integrated Into Complete Health Management
Optimal hormone levels support health and function, but hormones alone aren’t a complete longevity strategy. The most effective approach combines hormone optimization with body composition management through resistance training and adequate protein, metabolic health optimization addressing insulin resistance and visceral fat, cardiovascular risk management monitoring lipids and inflammation, sleep optimization supporting natural hormone production, and stress management preventing cortisol-driven hormone suppression. Our Pro Membership provides this comprehensive support—not just hormone prescriptions, but complete lifestyle and medical optimization guided by regular testing and physician supervision. This integrated approach produces better outcomes than hormone therapy alone.

Frequently Asked Questions About Hormone Optimization in Scottsdale
What hormones can be optimized and when is it appropriate?
We optimize testosterone (for men with confirmed low testosterone causing symptoms), estrogen and progesterone (for menopausal women), testosterone for women (when deficient and causing loss of libido or difficulty maintaining muscle), thyroid hormones (for subclinical or overt hypothyroidism), and DHEA (when significantly deficient). Hormone replacement is appropriate when blood testing confirms deficiency, symptoms correlate with low hormone levels, lifestyle optimization hasn’t resolved symptoms, no contraindications exist, and you’re willing to commit to ongoing monitoring. We don’t prescribe hormones to people with normal levels seeking enhancement, and we don’t treat hormones as anti-aging medicine for everyone—we address genuine deficiency causing symptoms or health issues.
How do you test for hormone deficiency?
Comprehensive hormone testing includes multiple markers providing complete picture. For testosterone assessment: total testosterone, free testosterone, sex hormone-binding globulin (SHBG), estradiol, luteinizing hormone (LH), follicle-stimulating hormone (FSH), and prolactin. For thyroid: TSH, free T4, free T3, reverse T3, and thyroid antibodies. For women approaching menopause: estradiol, progesterone, FSH, LH, and testosterone. For adrenal function: DHEA-S and potentially cortisol patterns. Testing must be done properly—morning samples for testosterone, repeat testing to confirm persistent deficiency, and interpretation in context of symptoms and clinical presentation. Single abnormal result doesn’t diagnose deficiency—we confirm through repeat testing before initiating therapy.
What are the benefits of testosterone replacement therapy for men?
When testosterone is genuinely deficient (consistently below 300-400 ng/dL) and causing symptoms, properly managed TRT provides significant benefits: improved energy and reduced fatigue within 3-6 weeks, enhanced mood and reduced depression within 3-6 weeks, increased libido and improved sexual function within 3-6 weeks to 3 months, increased muscle mass and strength over 3-12 months (with resistance training), reduced body fat particularly visceral fat over 3-12 months, improved bone density over 6-24 months, better insulin sensitivity and glucose metabolism, and improved overall quality of life. Benefits are dose-dependent to a point—achieving mid-normal levels (500-700 ng/dL) provides most benefits without increased side effect risks from supraphysiologic dosing.
What are the risks and side effects of testosterone therapy?
TRT is generally safe when properly monitored, but risks exist requiring awareness: polycythemia (elevated red blood cell count) is most common—requires monitoring hematocrit every 3-6 months, infertility is guaranteed—TRT suppresses sperm production (reversible when stopped but problematic if trying to conceive), sleep apnea can worsen particularly in overweight men, acne and oily skin occur in some men, gynecomastia (breast tissue development) if estradiol rises too high from testosterone conversion, testicular atrophy occurs (cosmetic, reverses if TRT stopped), and cardiovascular effects are debated—current evidence suggests TRT doesn’t increase cardiovascular risk when dosed appropriately in men with genuine deficiency. Regular monitoring minimizes risks—we check testosterone levels, estradiol, hematocrit, PSA, metabolic markers, and cardiovascular risk factors every 3-6 months.
How does hormone replacement work for women?
Menopausal hormone therapy addresses dramatic hormone declines women experience—estrogen, progesterone, and testosterone all drop at menopause causing significant symptoms. Standard HRT provides estrogen (and progesterone if uterus is intact) alleviating hot flashes, night sweats, mood changes, and bone loss. Adding testosterone—often overlooked—addresses persistent fatigue, complete loss of libido, difficulty maintaining muscle, and reduced vitality that estrogen alone doesn’t fully resolve. We use bioidentical hormones (chemically identical to hormones your body produces) at doses achieving physiologic levels. Delivery methods include transdermal creams or gels, patches, or pellets depending on individual needs. Regular monitoring ensures hormone levels are therapeutic but not excessive, and symptoms improve without side effects like excess facial hair or voice changes from testosterone doses that are too high.
What is thyroid optimization and who needs it?
Thyroid optimization addresses subclinical hypothyroidism and suboptimal thyroid function causing fatigue, weight gain, brain fog, depression, cold intolerance, and metabolic dysfunction. Standard testing (TSH only) misses many cases—comprehensive thyroid assessment includes TSH, free T4, free T3 (the active hormone), reverse T3 (inactive form that can block T3), and thyroid antibodies detecting autoimmune thyroid disease. Many people have “normal” TSH but low free T3 or high reverse T3 causing real symptoms. Thyroid hormone replacement options include levothyroxine (synthetic T4), liothyronine (synthetic T3), combination T4/T3 therapy, or natural desiccated thyroid. Proper dosing normalizes thyroid function, improves energy and metabolism, enhances cognitive function, and supports weight management.
How is Preamble different from TRT clinics?
Many TRT clinics prescribe testosterone after minimal testing (often just total testosterone), provide no comprehensive health assessment, use supraphysiologic doses creating artificially high levels, offer no meaningful monitoring beyond occasionally checking testosterone, and treat hormones in isolation from overall health. We take a medical approach: comprehensive testing before treatment including metabolic health, cardiovascular risk, and complete hormone panels, physician evaluation ensuring hormone replacement is appropriate and identifying contraindications, proper dosing achieving physiologic not supraphysiologic levels, regular monitoring every 3-6 months tracking hormone levels and critical safety markers (hematocrit, PSA, estradiol, metabolic markers), and integration with body composition tracking, metabolic optimization, and cardiovascular health management. This is hormone optimization as part of preventative medicine, not just hormone prescription.
Do you prescribe testosterone to women?
Yes, when clinically appropriate. Testosterone is critical for women’s health—affecting energy, libido, muscle mass, bone density, and mood—though at much lower levels than men. Women’s testosterone production drops 50% or more by menopause, and this contributes significantly to fatigue, complete loss of libido, difficulty maintaining muscle, and reduced vitality that estrogen replacement alone doesn’t fully address. We prescribe low-dose testosterone (typically 1-5mg daily via cream) for menopausal women with documented low testosterone and symptoms unresolved by estrogen replacement. Dosing must be carefully managed—too much causes virilization (voice deepening, facial hair, clitoral enlargement). Regular monitoring ensures levels are therapeutic (upper end of normal female range) without causing masculinizing side effects.
How long does hormone optimization take to work?
Timeline varies by hormone and outcome measured. For testosterone replacement in men: energy and mood improvements appear within 3-6 weeks, libido and sexual function improve within 3-6 weeks to 3 months, muscle mass gains occur over 3-12 months with proper training, body fat reduction happens over 3-12 months, and bone density improvement takes 6-24 months. For hormone replacement in women: hot flash relief often within days to weeks, mood and energy improvements within 2-6 weeks, libido improvement (if testosterone is included) within 4-8 weeks, and bone density protection over months to years. For thyroid optimization: energy improvements within 2-4 weeks as dose is optimized, metabolic improvements over 2-3 months, and cognitive function enhancement over weeks to months. Maximum benefits require 6-12 months of properly optimized hormone therapy.
Is hormone replacement therapy covered by insurance?
Coverage varies significantly. Some insurance covers testosterone replacement for men with documented deficiency below specific thresholds (often 300 ng/dL), though prior authorization is usually required. Menopausal hormone therapy (estrogen/progesterone) is often covered with similar authorization requirements. Thyroid hormone replacement for hypothyroidism is typically covered. However, comprehensive hormone optimization including regular monitoring, physician consultations, body composition tracking, and metabolic optimization through our Membership model is generally not covered as it’s preventative and optimization-focused rather than disease treatment. Our pricing is transparent and all-inclusive. All Preamble services are HSA/FSA eligible, allowing pre-tax dollars for hormone optimization.
What monitoring is required during hormone therapy?
Regular monitoring ensures hormone replacement is safe and effective. We recommend blood work every 3-6 months checking: hormone levels (testosterone, estradiol, thyroid hormones depending on what you’re taking) ensuring levels are optimal, hematocrit watching for polycythemia from testosterone, PSA monitoring prostate health in men on testosterone, liver function if using certain hormone formulations, lipid panels tracking cardiovascular effects, glucose and insulin assessing metabolic improvements, and other markers as clinically indicated. We also monitor symptoms—energy, mood, libido, sleep quality, body composition changes—adjusting doses based on both lab values and how you’re feeling. Between lab draws, we track body composition via DEXA showing muscle gain and fat loss objectively.
Where is hormone optimization provided?
All consultations, testing, monitoring, and medical supervision for hormone optimization happen at our Scottsdale clinic located at 16430 N Scottsdale Rd, Suite 110, Scottsdale, AZ 85254. Blood draws can be coordinated at convenient lab locations or arranged for in-home collection anywhere in the Phoenix metro area. Hormone prescriptions are sent to your preferred pharmacy. Follow-up consultations can be conducted in-person or virtually depending on your preference. We serve patients throughout Phoenix, Paradise Valley, Cave Creek, Fountain Hills, and surrounding communities who want physician-supervised hormone optimization, not just quick prescriptions from clinics with minimal medical oversight.
Optimize Your Hormones With Medical Supervision in Scottsdale
Stop accepting fatigue, declining muscle mass, low libido, and reduced vitality as inevitable aging. Comprehensive hormone testing reveals whether deficiency is contributing to symptoms, and physician-supervised hormone replacement restores function and quality of life when clinically appropriate.
Physician-supervised hormone optimization at our Scottsdale clinic
Comprehensive testing, proper dosing, and ongoing medical monitoring

