Your doctor tells you your BMI is 27, which puts you in the “overweight” category. You need to lose weight to improve your health.
But here’s what BMI can’t tell you: whether that extra weight is fat or muscle. Whether you’re carrying dangerous visceral fat around your organs or subcutaneous fat that’s relatively benign. Whether you’ve lost muscle mass over the years, which matters enormously for long-term health. Whether your bone density is declining and putting you at fracture risk.
BMI is a single number calculated from height and weight. It’s been the standard measure of healthy weight for decades because it’s easy to calculate and doesn’t require any special equipment. But easy doesn’t mean accurate, and it definitely doesn’t mean useful.
Body composition is what actually matters for health. How much fat are you carrying, where is that fat located, how much muscle mass do you have, and what’s happening with your bone density? These questions determine your metabolic health, your physical function, your disease risk, and your health trajectory as you age. BMI can’t answer any of them.
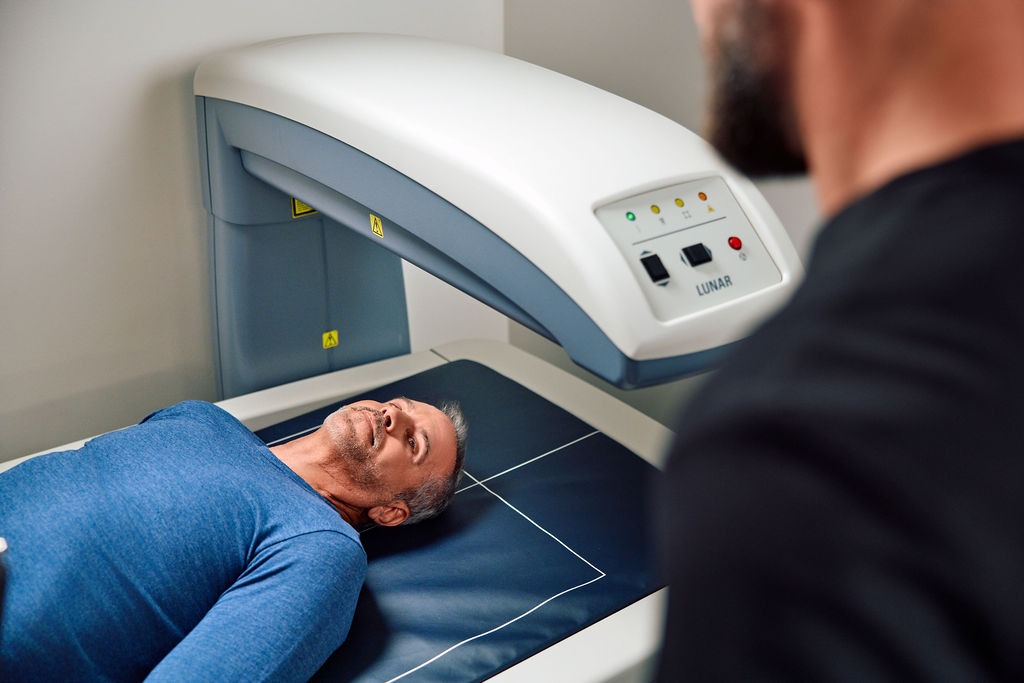
DEXA scans can. A DEXA scan takes 10 minutes, uses minimal radiation, and provides precise measurement of body fat percentage, lean muscle mass, bone density, and visceral fat. It’s the difference between knowing your weight and actually understanding your body composition.
So why does body composition matter more than weight? And when should you stop paying attention to BMI and start measuring what actually counts?
The BMI Problem: What It Measures and What It Misses
BMI (Body Mass Index) is calculated by dividing your weight in kilograms by your height in meters squared. A BMI under 18.5 is “underweight,” 18.5 to 24.9 is “normal weight,” 25 to 29.9 is “overweight,” and 30+ is “obese.”
This calculation has been used since the 1970s as a quick screening tool for population-level health assessment. It works reasonably well for sedentary populations where higher weight usually means higher body fat. But it breaks down completely when applied to individuals, especially active people with significant muscle mass.
The fundamental problem is that BMI doesn’t distinguish between fat mass and lean mass. A pound of muscle and a pound of fat both count the same in the calculation, even though they have completely different health implications. Muscle is metabolically active tissue that supports glucose metabolism, protects against injury, and maintains function as you age. Fat, particularly visceral fat, drives metabolic dysfunction and disease risk.
Consider someone who’s 5’10” and weighs 200 pounds. Their BMI is 28.7, which is “overweight” and approaching “obese.” But are they an athlete with 12% body fat and significant muscle mass, or are they sedentary with 30% body fat? BMI can’t tell you. The health implications of these two scenarios are completely different, but BMI categorizes them identically.
This isn’t a theoretical problem. Studies have found that up to 50% of people classified as “overweight” by BMI have metabolic health markers in the normal range, while 30% of people with “normal” BMI have metabolic dysfunction. BMI misclassifies metabolic health routinely because it doesn’t measure what actually matters.
The other thing BMI completely ignores is where fat is located. Subcutaneous fat (under the skin) is relatively benign. Visceral fat (around organs) drives insulin resistance, inflammation, and disease risk. Two people with identical BMI and even identical total body fat percentage can have vastly different health outcomes if one carries fat viscerally and the other doesn’t. BMI gives you no information about fat distribution.
BMI also tells you nothing about muscle mass or bone density, both of which are critical for healthspan. You could be losing muscle mass and bone density as you age, which dramatically increases your risk of falls, fractures, disability, and loss of independence, but as long as your weight stays stable, your BMI looks fine. This is particularly problematic for older adults, where maintaining muscle and bone matters more than weight.
What DEXA Scans Actually Measure
DEXA (Dual-Energy X-ray Absorptiometry) scans use low-dose x-rays at two different energy levels to differentiate between bone, lean tissue, and fat tissue. The scan takes about 10-20 minutes. You lie on a table fully clothed (no metal zippers or buttons) while the scanner passes over your body. The radiation exposure is minimal, equivalent to about one day of background radiation or a few hours on an airplane.
What you get from a DEXA scan is precise measurement of your body composition broken down into specific components.
Body fat percentage is the proportion of your total body weight that’s fat mass. For men, healthy ranges are roughly 10-20% depending on age and goals. For women, 20-30% is typical. DEXA measures this accurately to within about 1-2%, which is far more precise than bioelectrical impedance scales or other estimation methods. You can track changes over time and know definitively whether you’re losing fat or just losing weight (which could be water or muscle).
Lean body mass includes everything that isn’t fat or bone, primarily muscle but also organs and connective tissue. This number is critical because muscle mass determines your metabolic rate, your physical capacity, your glucose metabolism, and your ability to maintain independence as you age. Losing muscle mass (sarcopenia) is one of the most detrimental aspects of aging, and DEXA allows you to track whether you’re maintaining, building, or losing muscle over time.
Bone mineral density measures the strength and density of your bones. This is expressed as a T-score comparing your bone density to a healthy 30-year-old. A T-score above -1.0 is normal, -1.0 to -2.5 indicates osteopenia (low bone mass), and below -2.5 indicates osteoporosis. Low bone density dramatically increases fracture risk, particularly hip fractures in older adults, which often lead to permanent disability or death. Knowing your bone density allows intervention before fractures occur.
Visceral adipose tissue (VAT) measures fat around your organs in your abdominal cavity. This is the most metabolically harmful fat. Elevated visceral fat (generally above 100 square centimeters on DEXA) is strongly associated with insulin resistance, type 2 diabetes, cardiovascular disease, and inflammation regardless of your total body fat percentage. Two people with the same total body fat can have very different health profiles if one has high visceral fat and the other doesn’t.
Regional body composition breaks down your fat and lean mass by body region: arms, legs, trunk. This reveals patterns like losing muscle preferentially in the legs (common with aging and associated with mobility problems) or carrying excess fat in the trunk (associated with metabolic issues). Regional data helps target interventions more effectively.
All of this information comes from a single scan. Compare that to stepping on a scale, which gives you one number (total weight) that doesn’t tell you anything about what’s actually happening in your body.
Why Body Composition Matters More Than Weight
Your total body weight is a nearly meaningless number for health assessment. What matters is what that weight consists of and where it’s located. Here’s why body composition matters so much more than the number on the scale.
Metabolic health is determined by body composition, not weight. Insulin resistance, the root cause of type 2 diabetes and metabolic syndrome, is driven primarily by excess body fat, particularly visceral fat. But you can have elevated body fat with normal weight, or normal body fat with elevated weight if you carry significant muscle. BMI can’t distinguish these scenarios. Body composition can.
Studies have consistently shown that metabolically healthy obesity exists—people with elevated BMI but normal metabolic markers—and metabolically unhealthy normal weight exists—people with normal BMI but insulin resistance and other metabolic problems. Body composition explains this far better than BMI. It’s not about how much you weigh, it’s about how much fat you carry and where that fat is located.
Muscle mass determines your metabolic rate and glucose metabolism. Skeletal muscle is where glucose is primarily stored and used. More muscle mass means better glucose disposal and insulin sensitivity. It also means higher resting metabolic rate, making weight management easier. Losing muscle mass, which happens naturally with aging if you don’t actively maintain it, impairs metabolic function even if your weight stays stable. You could maintain the same weight from age 30 to 60 while losing 20 pounds of muscle and gaining 20 pounds of fat. Your BMI wouldn’t change, but your metabolic health would deteriorate dramatically.
Physical function and independence require muscle and bone. As you age, maintaining physical capacity means maintaining muscle strength and bone density. These determine whether you can climb stairs, carry groceries, recover from a fall, live independently, or require assistance with daily activities. Weight is irrelevant to these outcomes. A 70-year-old with low muscle mass and low bone density is at high risk for falls, fractures, and loss of independence regardless of whether their BMI is “normal.”
Cardiovascular disease risk is better predicted by body composition than BMI. Visceral fat is independently associated with cardiovascular risk. Total body fat percentage correlates with cardiovascular outcomes better than BMI. And low muscle mass in older adults predicts cardiovascular mortality independent of BMI. Body composition provides a more complete picture of cardiovascular risk than weight alone.
Athletic performance and body recomposition goals require composition data. If you’re strength training and trying to build muscle while losing fat, the scale might barely move even as your body composition improves dramatically. You could lose 10 pounds of fat, gain 8 pounds of muscle, and only see 2 pounds of weight loss. Without body composition data, you’d think you were failing when you’re actually succeeding. Athletes and active people need composition tracking, not weight tracking.
The Classic BMI Failures: Real-World Examples
BMI’s limitations aren’t theoretical. They create real problems in clinical practice and mislead people about their health constantly.
The muscular athlete who strength trains regularly might be 5’9″ and 190 pounds with 10% body fat and exceptional metabolic health. Their BMI is 28, categorizing them as overweight and suggesting they need to lose weight for health. Losing weight would mean losing muscle, which would actually harm their health. BMI gives exactly the wrong recommendation.
The sedentary person with normal weight obesity might be 5’9″ and 150 pounds with 28% body fat and low muscle mass. Their BMI is 22, perfectly “normal,” so they’re told they’re healthy. But they have insulin resistance developing, low cardiovascular fitness, and are at risk for metabolic disease. BMI provides false reassurance.
The older adult losing muscle might maintain stable weight from age 50 to 70 while losing significant muscle mass and gaining fat mass. Their BMI stays in the normal range the entire time, but their body composition has shifted in ways that dramatically increase their risk of falls, fractures, disability, and metabolic disease. BMI misses the entire problem.
The person with high visceral fat might have normal total body fat percentage but store fat disproportionately in the abdominal cavity around organs. This creates significant metabolic risk even with normal BMI and normal total body composition. Only measuring visceral fat specifically reveals this risk.
These aren’t edge cases. They represent common patterns that BMI handles poorly or completely misses.
When DEXA Scans Are Most Valuable
DEXA scans aren’t necessary for everyone, but they’re extremely valuable in specific situations where body composition data changes decision-making.
If you’re actively working to change body composition through strength training, targeted fat loss, or athletic performance, DEXA provides objective feedback on whether your approach is working. Are you actually building muscle? Is the weight you’re losing fat or muscle? Is your visceral fat decreasing? These answers guide programming and prevent wasted effort.
For people over 40, especially women approaching or past menopause, DEXA reveals whether you’re maintaining muscle and bone as you age. Muscle loss accelerates after 40 without resistance training. Bone density declines, particularly in women after menopause. Catching these declines early allows intervention before they become serious problems.
If you have metabolic concerns like prediabetes, insulin resistance, or family history of type 2 diabetes, knowing your visceral fat and total body fat percentage provides additional context for metabolic risk and tracks whether interventions are working. You might not lose much total weight improving metabolic health, but visceral fat should decrease, and you can track that with DEXA.
Anyone with “normal” BMI but metabolic issues benefits from body composition assessment. If your BMI looks fine but you have elevated glucose, cholesterol problems, or other metabolic markers, DEXA might reveal that you have normal weight obesity or elevated visceral fat that explains the disconnect.
People who have lost significant weight and want to maintain their results benefit from DEXA by tracking whether they’re maintaining muscle mass during maintenance. Weight loss often includes both fat and muscle loss. Maintaining weight without regaining fat while preserving muscle requires monitoring composition, not just weight.
Athletes and serious exercisers use DEXA to track training adaptations, optimize body composition for performance, and ensure training programs are producing desired results. For sports with weight classes or aesthetic components, composition matters far more than weight.
What to Do With Your DEXA Results
Getting a DEXA scan is only valuable if you understand the results and use them to guide decisions. Here’s what to look for and what actions different findings suggest.
If your body fat percentage is elevated (above 25% for men or 35% for women, though optimal ranges vary), focus on fat loss through caloric deficit, high-protein diet, and resistance training to preserve muscle. Track progress with repeat DEXA every 3-6 months to ensure you’re losing fat without losing significant muscle.
If your muscle mass is low for your age and size, prioritize resistance training with progressive overload and adequate protein intake (roughly 0.7-1 gram per pound of body weight). This is particularly critical if you’re over 50, where muscle loss accelerates without intervention. Retest in 6-12 months to confirm you’re building muscle.
If your visceral fat is elevated (above 100 square centimeters), this requires aggressive metabolic intervention even if your total body fat seems acceptable. Reduce refined carbohydrates and added sugars, increase physical activity especially resistance training and higher-intensity cardio, and consider comprehensive metabolic blood work to assess insulin resistance. Visceral fat is particularly responsive to lifestyle changes.
If your bone density shows osteopenia or osteoporosis (T-score below -1.0), you need intervention to prevent fractures. Weight-bearing exercise and resistance training help maintain and potentially build bone density. Ensure adequate calcium (1000-1200mg daily from food and supplements) and vitamin D (blood levels should be 40-60 ng/mL). Severe cases might require medication, which your physician can discuss.
If your body composition is already optimal but you want to maintain it as you age, retest annually to catch any declines early. Maintaining good composition is easier than regaining it after loss.
The Bottom Line: Measure What Matters
BMI was created as a population-level statistical tool in the 1800s. It’s still useful for population health research, but it’s a terrible tool for assessing individual health. It doesn’t measure what actually determines metabolic health, physical function, or disease risk.
Body composition does. How much fat you carry, where that fat is located, how much muscle mass you have, and your bone density all directly determine health outcomes in ways that total body weight simply doesn’t.
DEXA scans provide this information accurately and precisely in a quick, low-radiation test that you can repeat periodically to track changes. If you’re serious about understanding your body and optimizing health, stop stepping on the scale obsessively and get a DEXA scan. Measure what actually matters.
Your weight is just a number. Your body composition is your health.

Get Accurate Body Composition Analysis at Preamble Health
DEXA scans are a core component of our comprehensive health assessments at Preamble Health. We use hospital-grade DEXA technology to provide precise body composition data that guides personalized recommendations for nutrition, training, and health optimization.
Whether you’re working on fat loss, building muscle, tracking metabolic health, or monitoring bone density as you age, DEXA provides the objective data you need to make informed decisions and track progress.
Ready to measure what actually matters?
- Schedule a DEXA scan at our Scottsdale location
- Learn about our Executive Physical which includes DEXA and comprehensive health assessment
- Book a consultation to discuss your body composition goals
- Read our complete DEXA scan guide for more detailed information
Related resources:
- What is Medicine 3.0? discussing our data-driven approach to health optimization
- Healthspan vs Lifespan exploring why physical function matters more than just longevity
- Advanced Blood Work Guide for metabolic health assessment beyond body composition