Here’s a scenario most people experience: You go to your annual physical. Your doctor orders basic blood work, spends 15 minutes with you, tells you everything looks fine, and sends you on your way. Cost: maybe $200-300 if you’re paying out of pocket, often covered by insurance.
Then someone mentions they spent $3,000 on a comprehensive executive physical—multiple hours of testing, detailed metabolic assessment, body composition analysis, cardiovascular fitness testing, extended consultation with a physician focused on prevention.
Your immediate thought: “That’s way too expensive. My annual physical is fine.”
But is it? What is that $3,000 actually buying compared to the standard $200 checkup? More importantly, what’s the cost of not investing in comprehensive preventative healthcare?
These are the questions most people don’t ask, but they matter enormously. Because the real comparison isn’t between spending $3,000 on prevention versus spending nothing. It’s between spending $3,000 on prevention versus spending tens or hundreds of thousands managing preventable disease for decades.
When you frame it that way, the calculation looks very different.
Premium preventative healthcare—comprehensive assessments, advanced testing, optimization rather than just disease screening—requires upfront investment. It’s not cheap. But neither is managing diabetes for 30 years, recovering from a heart attack, or dealing with complications from preventable disease.
So let’s do the math. What does prevention actually cost? What does disease cost? And for whom does investing in premium preventative healthcare make sense?
What Premium Preventative Healthcare Actually Includes
First, let’s define what we’re talking about. “Premium preventative healthcare” isn’t a standard term, but it generally means comprehensive health assessment and optimization beyond what standard annual physicals provide.
Standard Annual Physical (What Most People Get)
A typical annual physical includes:
- Brief medical history review
- Vital signs (blood pressure, heart rate, temperature)
- Basic physical exam
- Standard blood work (10-15 markers)
- Maybe screening tests appropriate for your age (colonoscopy, mammogram, etc.)
- 15-20 minutes with your doctor
Total time investment: maybe an hour including the blood draw. Cost: $200-400 if self-paying, often covered by insurance with copay.
This screening is valuable for catching obvious disease. If you have high blood pressure, diabetes, or other detectable conditions, a standard physical will likely identify them.
But it’s not designed to:
- Detect early metabolic dysfunction before disease develops
- Assess cardiovascular fitness or physical capacity
- Optimize metabolic health and body composition
- Provide detailed disease risk assessment
- Create personalized prevention strategies
It’s reactive screening (catching disease after it develops) rather than proactive prevention (maintaining health so disease doesn’t develop).
Premium Preventative Healthcare (The Comprehensive Approach)
Premium preventative healthcare—whether it’s an executive physical, concierge medicine, or Medicine 3.0 approach—includes substantially more:
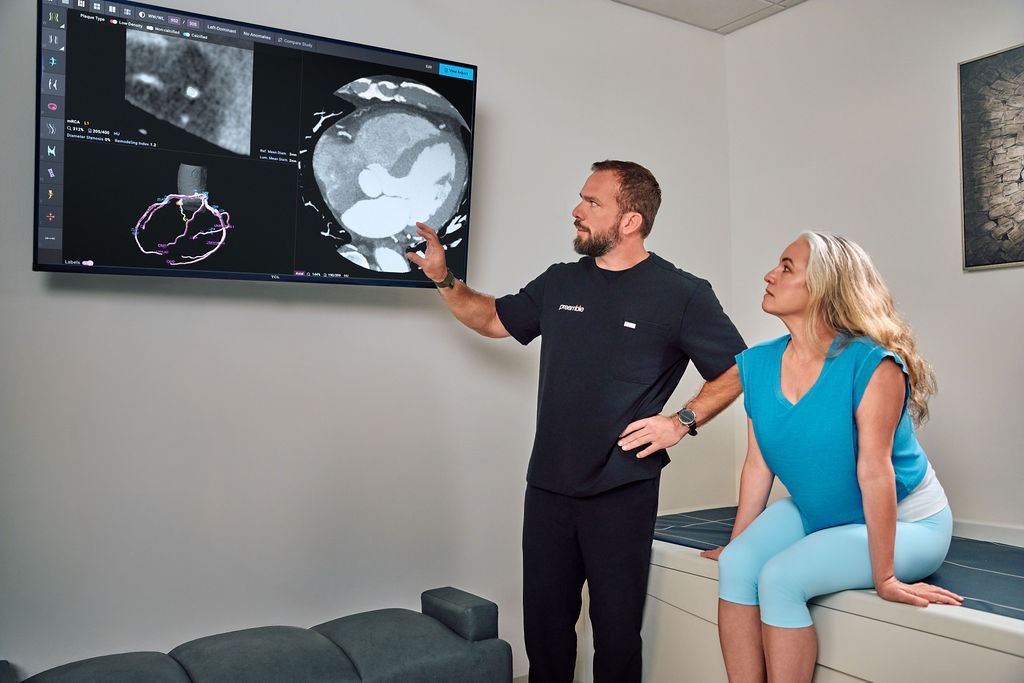
Advanced Blood Work – 100+ markers including detailed metabolic assessment, advanced lipid panels, inflammation markers, hormone testing, and nutrient status. This reveals early metabolic dysfunction, cardiovascular risk factors, and optimization opportunities that standard panels miss. (See our detailed blood work guide)
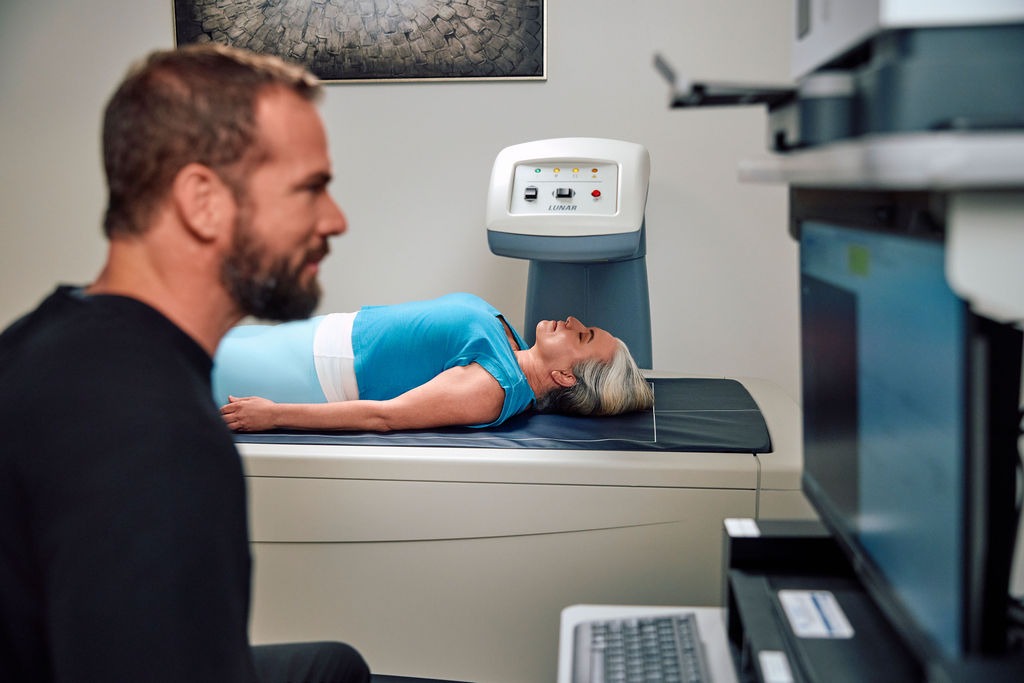
Body Composition Analysis – DEXA scans measuring body fat percentage, lean muscle mass, bone density, and visceral fat. This provides objective data on body composition rather than just weight and BMI. (Learn about DEXA scans)
Cardiovascular Fitness Testing – VO2 max testing measuring actual cardiovascular fitness, which is one of the strongest predictors of longevity. Standard physicals don’t assess this at all. (Read about VO2 max testing)
Extended Time with Physician – 60-90+ minutes discussing results, health goals, family history, and creating personalized recommendations. This is actual health optimization, not just “everything looks fine, see you next year.”
Personalized Prevention Plan – Specific, actionable recommendations for nutrition, exercise, supplementation, and lifestyle based on your actual data rather than generic guidelines.
Ongoing Support – Some programs include regular check-ins, access to healthcare providers between visits, and continued optimization rather than just annual assessment.
Total time investment: 3-6 hours for comprehensive assessment. Cost: $1,500-$10,000 depending on comprehensiveness, typically $2,000-$4,000 for a thorough executive physical.
This is substantially more expensive upfront. The question is whether it’s worth it.
The Real Cost of Preventable Disease
To understand whether prevention is worth the investment, you need to understand what you’re preventing—and what that prevention is worth.
Type 2 Diabetes: The Preventable Epidemic
Type 2 diabetes is overwhelmingly preventable through maintaining metabolic health. Yet it affects over 37 million Americans, with another 96 million having prediabetes. Most will develop diabetes without intervention.
The costs of diabetes:
Direct medical costs average $9,600 per year for people with diabetes (American Diabetes Association data). Over 20 years, that’s $192,000. Over 30 years, $288,000.
But direct costs understate the true burden:
- Lost productivity and reduced income
- Complications: kidney disease requiring dialysis ($90,000+ annually), neuropathy, vision loss, amputation, cardiovascular disease
- Reduced quality of life and independence
- Cognitive decline (diabetes increases dementia risk significantly)
The lifetime cost of diabetes starting at age 50 is estimated at $300,000-500,000 when you include complications and indirect costs.
The cost of prevention:
Diabetes is prevented by maintaining metabolic health—healthy diet, regular exercise, healthy weight. Detecting insulin resistance early (through comprehensive blood work that tests fasting insulin, not just glucose) allows intervention before diabetes develops.
Cost to detect early: $500-1,000 for comprehensive metabolic testing. Cost to reverse prediabetes: primarily time investment in dietary changes and exercise, maybe $1,000-2,000 in gym memberships or nutritionist consultations if needed.
Total prevention investment: $2,000-3,000 upfront, plus ongoing lifestyle habits that improve overall health beyond just diabetes prevention.
The ROI is obvious: spend $2,000-3,000 to prevent $300,000-500,000 in disease costs.
Cardiovascular Disease: The #1 Killer
Heart disease is the leading cause of death in the US. Much of it is preventable through managing risk factors—cholesterol, blood pressure, inflammation, metabolic health, physical fitness.
The costs of cardiovascular disease:
A heart attack costs $50,000-100,000+ for acute treatment. If you need bypass surgery or stent placement, add another $70,000-200,000. Ongoing medication and monitoring costs $5,000-10,000 annually.
Stroke costs are similar: $75,000-150,000 for acute treatment, plus potentially long-term disability requiring ongoing care at $50,000-100,000+ annually.
And these costs assume recovery. Many people don’t fully recover—they live with reduced function, disability, inability to work, and dramatically compressed healthspan (see our article on healthspan vs lifespan).
The cost of prevention:
Cardiovascular disease prevention requires:
- Knowing your risk factors (comprehensive lipid testing measuring ApoB and LDL particle number, not just basic cholesterol)
- Maintaining cardiovascular fitness (VO2 max testing reveals actual fitness level)
- Managing blood pressure and inflammation
- Maintaining healthy body composition
Comprehensive cardiovascular risk assessment: $800-1,500. Interventions: primarily exercise and nutrition, with medication if needed (statins cost $10-50/month for generics).
Total prevention investment: $1,500-3,000 upfront, plus lifestyle habits.
The ROI: spend $2,000-3,000 to dramatically reduce risk of $200,000+ in treatment costs, potential disability, and years of compressed healthspan.
Cancer: Earlier Detection Saves Lives and Costs
While not all cancers are preventable, many are influenced by lifestyle factors (obesity, smoking, alcohol, diet, physical inactivity). And early detection dramatically improves outcomes and reduces treatment costs.
The costs of cancer treatment:
Average cancer treatment costs $150,000-300,000, with many cancers costing substantially more. Novel immunotherapies can cost $100,000-500,000 per year. Chemotherapy, radiation, surgery, ongoing monitoring—costs add up quickly.
Beyond direct costs, cancer treatment often means loss of income, reduced quality of life during treatment, and potential long-term complications.
The cost of prevention and early detection:
Cancer prevention involves lifestyle factors (maintaining healthy weight, not smoking, limiting alcohol, regular exercise) plus age-appropriate screening (colonoscopy, mammography, etc.).
Comprehensive preventative healthcare emphasizes these behaviors and ensures appropriate screening happens on schedule rather than getting missed or delayed.
While you can’t prevent all cancers, reducing risk and catching cancers early when they’re most treatable substantially reduces costs and improves outcomes.
The Pattern: Prevention Is Cheap, Disease Is Expensive
This pattern repeats across chronic diseases:
Osteoporosis – DEXA scans ($100-150) detect low bone density early, allowing intervention with weight-bearing exercise, vitamin D, and possibly medication. Hip fractures cost $40,000-100,000 and often result in permanent disability in older adults.
Sarcopenia (muscle loss) – Strength training maintains muscle mass ($50-100/month gym membership). Loss of muscle leads to falls, fractures, loss of independence, nursing home placement ($80,000-100,000 annually).
Cognitive decline – Maintaining cardiovascular fitness, managing metabolic health, staying socially engaged, and exercising regularly all reduce dementia risk. Alzheimer’s care costs $250,000-400,000 over the course of the disease.
In every case, prevention costs a fraction of treatment. And prevention provides the additional benefit of maintained healthspan—you’re not just avoiding disease costs, you’re maintaining quality of life.
The ROI Calculation: When Does Prevention Pay Off?
So if prevention is dramatically cheaper than disease treatment, when does investing in premium preventative healthcare make financial sense?
The Simple Math
Let’s use conservative estimates:
Scenario 1: Standard Healthcare
- Annual physical: $300/year (often covered by insurance)
- Standard blood work and basic screening
- Wait for disease to develop, then manage it
- Assume 40% chance of developing at least one major chronic disease (diabetes, heart disease, cancer) over 30 years based on population averages
- Average lifetime cost of chronic disease management: $250,000
Expected lifetime healthcare cost: ($300 × 30 years) + (0.4 × $250,000) = $109,000
Scenario 2: Premium Preventative Healthcare
- Comprehensive assessment every 2-3 years: $2,750 + cost of membership
- Annual follow-up with advanced blood work: $800/year
- Gym membership and health-supporting behaviors: $1,200/year
- Assume prevention reduces chronic disease risk from 40% to 15% through early detection and intervention
- Average lifetime cost of chronic disease if it does develop: $150,000 (caught earlier, less severe)
Expected lifetime healthcare cost: ($2,500 × 10 assessments) + ($800 × 30 years) + ($1,200 × 30 years) + (0.15 × $150,000) = $107,500
The financial outcomes are nearly identical, but Scenario 2 includes:
- 25 percentage point reduction in chronic disease risk (40% to 15%)
- Earlier detection if disease does develop (better outcomes, lower costs)
- Maintained healthspan and quality of life
- Regular exercise and healthy lifestyle that provides benefits beyond just disease prevention
And these numbers underestimate the value of prevention because they don’t account for:
- Lost income due to disease or disability
- Quality of life during disease management
- Caregiver burden on family
- Reduced healthspan in final years
When Prevention Has the Highest ROI
Premium preventative healthcare provides the most value for:
People with elevated risk – Family history of heart disease, diabetes, cancer, or other chronic disease substantially increases your risk. If your baseline risk is 60% instead of 40%, prevention’s ROI increases dramatically.
People in their 40s-60s – This is the optimal intervention window. You’re old enough that risk factors are developing, but young enough that interventions are highly effective. Catching metabolic dysfunction at 45 prevents decades of disease.
High earners – If you make $150,000+, lost income due to disease or disability creates significant financial cost beyond medical expenses. Maintaining health protects your earning capacity.
People who value quality of life – If maintaining independence and physical capacity matters to you, prevention’s value extends beyond just financial ROI. The ability to travel, pursue hobbies, and remain active is worth more than money to many people.
Those with limited family medical history knowledge – If you don’t know your family history (adopted, estranged family, etc.), comprehensive assessment provides baseline data you don’t have from family history.
When Standard Healthcare Might Be Sufficient
Premium preventative healthcare might not be necessary if:
You’re already very healthy with low risk – If you’re under 35, very active, healthy weight, no family history of chronic disease, and no risk factors, comprehensive assessment might not reveal anything actionable. Standard screening is probably sufficient until risk increases with age.
You can’t afford it without sacrificing basics – If paying $2,750 for a comprehensive assessment means not paying rent or buying food, obviously don’t do it. Health requires resources, and if those resources are limited, prioritize basics (housing, food, regular exercise, adequate sleep) before comprehensive testing.
You’re already doing everything right – If you’re maintaining excellent health behaviors (regular exercise, healthy diet, healthy weight, good sleep), standard screening might be sufficient to confirm you’re on track. Though even health-conscious people often discover optimization opportunities through comprehensive testing.
What You’re Really Paying For
Beyond the specific tests and assessments, premium preventative healthcare provides several less tangible benefits worth considering.
Early Detection When Intervention Is Most Effective
Most chronic diseases develop over decades. There’s a window—sometimes 5-10 years—where dysfunction is present but disease hasn’t been established yet. This is the optimal intervention window.
Standard healthcare often catches problems after this window closes. Your fasting glucose finally hits 126 mg/dL (diabetes diagnosis), but you’ve had insulin resistance and gradually rising glucose for 10 years. By the time you’re diagnosed, beta cell function has declined substantially.
Comprehensive testing catches problems in that earlier window when intervention is highly effective. Your fasting insulin is elevated at 45 years old, glucose is 92 mg/dL (still “normal”), and you have 10+ years to reverse course before diabetes develops.
That early detection window is enormously valuable but hard to quantify financially.
Personalized Rather Than Generic Advice
Standard healthcare provides population-level recommendations: eat healthy, exercise more, lose weight if overweight. These are fine guidelines, but they’re generic.
Comprehensive assessment with detailed testing provides personalized recommendations based on your actual data:
- Your LDL cholesterol is “normal” but your ApoB is elevated—you need aggressive LDL management
- Your fasting glucose is fine but your insulin is high—you need to focus on insulin sensitivity
- Your cardiovascular fitness is low for your age—specific VO2 max targets for improvement
- You have vitamin D deficiency causing fatigue—specific supplementation dose
This personalization makes interventions more effective because they target your actual issues rather than general recommendations.
Accountability and Ongoing Optimization
Having objective data creates accountability. You can’t fool a DEXA scan or VO2 max test. If you haven’t been maintaining muscle mass or cardiovascular fitness, your results will show it.
This accountability drives behavior change more effectively than vague goals like “get healthier.”
Additionally, retesting every 1-2 years shows whether your interventions are working. Your fasting insulin decreased, your VO2 max improved, your body composition shifted—objective confirmation you’re on the right track. Or if results haven’t improved, you know you need to adjust your approach.
Peace of Mind
For some people, comprehensive testing provides psychological value through peace of mind. You’re not wondering if something’s wrong—you have data showing you’re healthy (or showing exactly what needs improvement).
This is particularly valuable if you have anxiety about health or if you have strong family history of disease and want confirmation you’re not developing similar problems.
How to Get Started with Prevention (Without Spending $10,000)
If you’re convinced prevention is valuable but aren’t ready to spend thousands on comprehensive assessment, you can take incremental steps.
Start with the Basics
Before spending money on advanced testing, implement basic health behaviors:
Exercise regularly – Both cardiovascular exercise and strength training. This is the highest-value health intervention available, and it’s essentially free (or gym membership costs $30-100/month).
Eat mostly whole foods – Emphasize vegetables, adequate protein, healthy fats, whole grains if you tolerate them. Minimize processed foods, added sugars, and excessive refined carbohydrates.
Maintain healthy weight – If you’re significantly overweight, losing even 5-10% of body weight improves metabolic health substantially.
Prioritize sleep – Aim for 7-9 hours consistently. This costs nothing and affects everything else.
Don’t smoke, limit alcohol – Obvious but worth stating.
These behaviors prevent most chronic disease and don’t require expensive testing or assessments. They’re the foundation everything else builds on.
Add Targeted Testing
Once basics are in place, add specific testing to identify issues:
Comprehensive blood work – This is the highest-value testing for most people. Advanced metabolic panels ($300-800) reveal insulin resistance, cardiovascular risk, inflammation, and nutrient deficiencies that standard panels miss. (Learn what’s included)
Body composition analysis – DEXA scan ($100-150) provides objective data on body fat, muscle mass, and bone density. This is much more informative than just weight or BMI.
Cardiovascular fitness testing – VO2 max test ($150-250) measures actual fitness level and provides training targets. This is particularly valuable if you’re exercising regularly but want to know if your fitness is optimal.
Total cost for these three categories: $550-1,200. This covers most of what comprehensive assessment provides without the full executive physical price tag.
Work with Prevention-Focused Providers
Not all healthcare providers focus on prevention and optimization. Many are trained in disease management—treating problems after they develop.
Look for providers who:
- Emphasize prevention rather than just treating disease
- Use optimal ranges rather than just reference ranges for lab interpretation
- Spend adequate time discussing lifestyle interventions
- Order comprehensive testing rather than just basic panels
- Help you track progress over time
This might be a functional medicine practitioner, a preventative cardiologist, a physician practicing Medicine 3.0, or a well-informed primary care doctor. The specific credentials matter less than the philosophy and approach.
Retest Annually or Every 2 Years
Prevention isn’t one-and-done. Retest periodically (annually if you’re actively working to improve specific markers, every 2-3 years for maintenance) to track trends.
This ongoing monitoring shows whether you’re maintaining health as you age or whether issues are developing that need intervention.
The Bottom Line: Prevention Is Worth It
Is premium preventative healthcare worth the investment? For most people over 40, especially those with elevated risk or who prioritize long-term health, yes—absolutely.
The financial ROI is clear: spending $2,000-5,000 annually on prevention costs far less than spending $200,000-500,000 managing preventable chronic disease for decades. Even if prevention only reduces your disease risk by 20-30%, it pays for itself many times over.
But the real value extends beyond financial ROI:
- Maintained healthspan and quality of life
- Independence and physical capability as you age
- Peace of mind from knowing your health status
- Early detection when intervention is most effective
- Personalized optimization rather than generic recommendations
Prevention requires upfront investment—both financial and time. It requires prioritizing future health over current convenience. But the alternative is waiting for disease to develop, then managing it for the rest of your life at far greater financial and personal cost.
The question isn’t whether you can afford to invest in prevention. It’s whether you can afford not to.
Invest in Prevention at Preamble Health
At Preamble Health, we believe prevention is always less expensive and more effective than treatment. Our Medicine 3.0 approach focuses on maintaining health and preventing disease rather than waiting to manage it after it develops.
Our comprehensive assessments—including advanced blood work, VO2 max testing, DEXA scans, and extended physician consultation—provide the detailed information you need to optimize your health trajectory.
Our programs:
Core Membership ($650) – Advanced blood work with 100+ markers, detailed interpretation, and personalized recommendations. Ideal for metabolic health assessment and optimization.
Medicine 3.0 Executive Physical ($2,750) – Comprehensive assessment including all testing, extended physician time, and complete prevention plan. Designed for people serious about long-term health optimization.
Ready to invest in your health?
- Schedule a consultation to discuss which program fits your goals
- Learn about our Medicine 3.0 Executive Physical
- Explore our Core Membership
- Read about our Medicine 3.0 philosophy
Related resources:
- What is Medicine 3.0? – Our approach to proactive prevention
- Healthspan vs Lifespan – Why living well matters more than living long
- Advanced Blood Work Guide – What comprehensive testing reveals
- Who Needs Comprehensive Preventative Health Screening?




